Behavioural Supports Ontario (BSO) provides behavioural health care services for older adults in Ontario with, or at risk of, responsive behaviours/personal expressions associated with dementia, complex mental health, substance use and/or other neurological conditions. BSO also provides support to family care partners and healthcare providers across sectors.
BSO was implemented in 2012 to leverage existing resources and enhance coordination across the continuum of care. All long-term care (LTC) homes in Ontario have access to specialized behavioural support resources either through BSO team members that work in their LTC home or through a mobile team. BSO teams are also available to people living in the community, including private dwellings, assisted living, retirement homes, etc., and some of Ontario’s hospitals also have BSO team members.
Although BSO models (i.e., team structures) look different across Ontario, all BSO teams are united under common mandate, principles, framework of care and standards of practice.
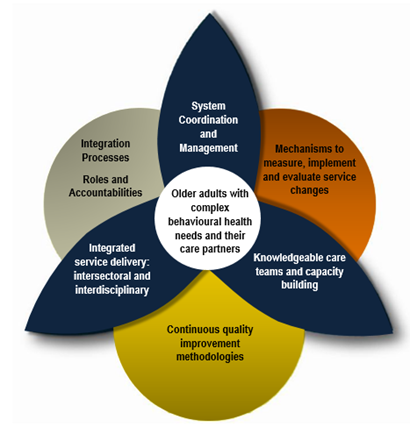
BSO Provincial Framework of Care & Principles
BSO’s framework of care is modeled under three provincial pillars:
Pillar 1: System Coordination and Management
Pillar 2: Integrated Service Delivery - Intersectoral and Interdisciplinary
Pillar 3: Knowledgeable Care Team and Capacity Building
BSO is rooted in person and family-partnered care and is guided by seven value-based principles:
1) Behaviour is communication
Responsive behaviours/personal expressions can be minimized by understanding the person and adapting the environment or care to better meet the individual’s unmet needs. Behaviours are not meaningless; they are an attempt to express distress, problem-solve or communicate unmet needs.
2) Respect
All persons are treated with respect and accepted as they are. Respect and trust characterize the relationships between clinicians and individuals/family care partners, and between providers across systems.
3) Diversity
Practices value the language, ethnicity, race, religion, gender, beliefs/traditions, and life experiences of the people being served.
4) Collaborative Care
Accessible, comprehensive assessment and intervention require an interdisciplinary approach that includes professionals from different disciplines, as well as the individuals/family care partners, to cooperatively create a joint, single plan of care.
5) Safety
The creation of a culture of safety and well-being is promoted where older adults and families live and visit and where staff work.
6) System Coordination & Integration
Systems are built upon existing resources and initiatives and encourage the development of synergies among existing and new partners to ensure access to a full range of integrated services and flexible supports based on need.
7) Accountability & Sustainability
The accountability of the system, health, and social service providers to funders and to each other is defined and ensured (Ontario Behavioural Support System Project, 2010).

Behavioural Support Transition Units
BSTUs provide specialized care to individuals with responsive behaviours/personal expressions that cannot be effectively supported in their current environment and other services have been explored.